Get Back to the Life You Were Built For.
Evaluation and treatment for mitochondrial dysfunction. Addressing fatigue, brain fog, metabolic decline, and chronic illness at the cellular level. Serving patients throughout Dallas, DFW, Irving, and Las Colinas.

Schedule a Free Consultation with Our New Patient Coordinator:
Or fill in the Inquiry Form below, and we will contact you.
Why Mitochondrial Health Matters
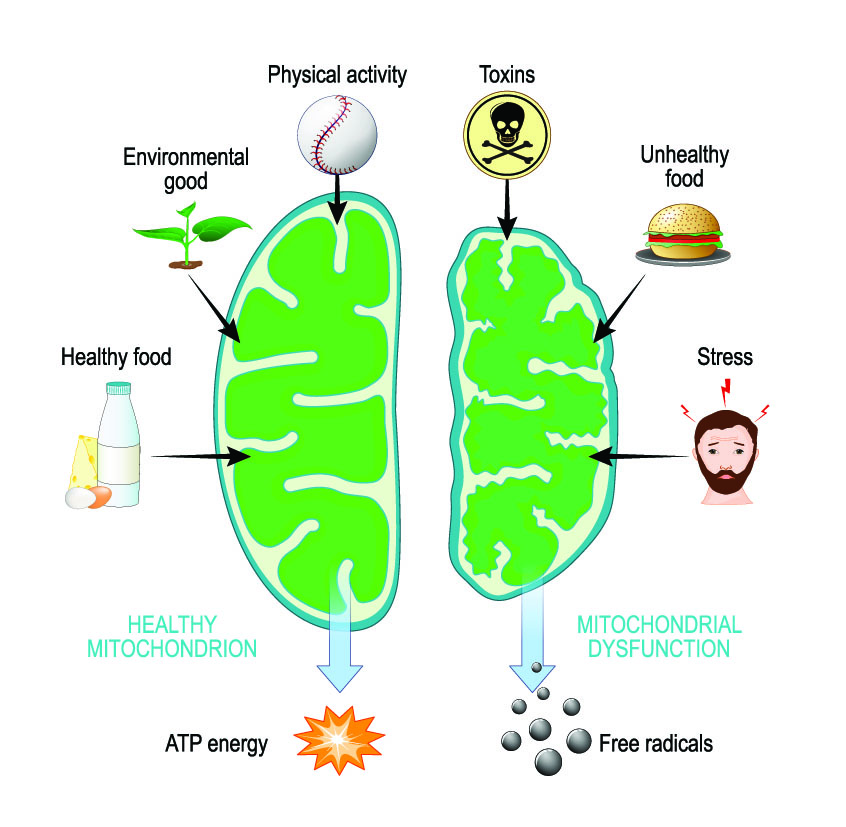
Mitochondria are the energy-producing structures inside your cells. They take in nutrients and oxygen and convert them into ATP (adenosine triphosphate)—the fuel that powers every biological process in the body. The heart, brain, and muscles rely most heavily on mitochondria, as these organs and tissues have the highest energy demands.
When mitochondria are damaged or underperforming, the effects are felt throughout the body. Poor cellular energy production is now recognized as a common underlying factor in many chronic diseases—and one of the most overlooked causes of persistent fatigue, cognitive decline, and metabolic dysfunction.
For patients in the Dallas and Las Colinas area who have been dealing with unexplained fatigue, brain fog, or chronic symptoms that have not responded to conventional treatment, mitochondrial health is often a significant piece of the puzzle.
What Damages Mitochondria?
Mitochondrial decline is a natural part of aging, but it can be accelerated by a range of environmental and lifestyle factors, including:
- Chronic stress
- Poor sleep quality or insufficient sleep
- A diet high in refined sugar and processed foods
- Environmental toxins and pollutants
- Sedentary lifestyle
- Nutritional deficiencies
- Chronic inflammation
Mitochondria also produce a byproduct called reactive oxygen species (ROS), a type of free radical. When antioxidant intake is insufficient or antioxidant production declines with age, these free radicals can accumulate and damage mitochondria, creating a cycle of worsening cellular dysfunction.
Conditions Linked to Mitochondrial Dysfunction
Because all cellular processes depend on energy, poor mitochondrial function is a common denominator in a wide range of chronic diseases. Conditions that have been linked to mitochondrial dysfunction include:
• Chronic fatigue syndrome
• Fibromyalgia
• Insulin Resistance and Type 2 Diabetes
• Obesity and metabolic syndrome
• Cardiovascular disease
• Fatty liver disease
• Alzheimer’s disease and cognitive decline
• Parkinson’s disease
• Depression and bipolar disorder
• Multiple sclerosis
• Inflammatory bowel disease
• Chronic kidney disease
• Autoimmune conditions
• Skin disorders
• Infertility and reproductive concerns
The breadth of this list reflects a fundamental reality: when cells cannot produce adequate energy, virtually every system in the body is affected.
Schedule a Free Consultation with Our New Patient Coordinator:
Or fill in the Inquiry Form below, and we will contact you.
The Thyroid-Mitochondria Connection
Thyroid hormone T3 (triiodothyronine) is one of the primary regulators of mitochondrial activity. It influences metabolic rate, brain function, heart and digestive health, muscle control, and bone maintenance. When T3 levels are adequate, mitochondria produce energy efficiently. When T3 is reduced or absent, mitochondrial energy production declines, and mitochondria can eventually die.
The reverse is equally important: when mitochondria are damaged by toxins, chronic stress, or oxidative stress, the thyroid loses its ability to produce adequate hormone levels. Reduced thyroid hormone further impairs mitochondrial function. It becomes a self-reinforcing cycle that is difficult to resolve without addressing both systems together.
This is why a comprehensive thyroid evaluation—not just a TSH test—is essential for assessing mitochondrial health. Our providers are experienced in diagnosing and treating the full spectrum of thyroid dysfunction, including cases where standard labs appear normal.
The Gut-Mitochondria Connection
The relationship between gut health and mitochondrial function is an emerging and important area of functional medicine research.
In the gut, the cells lining the intestinal wall — and their mitochondria — exist in close proximity to the bacteria that make up the gut microbiome. These bacteria interact with the body’s cells largely through mitochondrial pathways. Research suggests that a healthy, diverse gut microbiome supports healthy mitochondrial function, while gut dysbiosis — an imbalance of beneficial to harmful bacteria — creates a state of chronic inflammation that directly impairs mitochondrial processes.
Chronic gut inflammation acts as a persistent drain on the body’s cellular energy systems, compounding mitochondrial dysfunction and its downstream effects on hormones, metabolism, and overall health.
Supporting Mitochondrial Health
Alongside clinical treatment, the following lifestyle practices support mitochondrial function and help reduce oxidative damage:
Eat a whole-food, plant-rich diet high in antioxidants and phytonutrients—vegetables, fruits, nuts, seeds, beans, and whole grains.
- Eliminate processed foods, refined sugar, and trans fats.
- Increase omega-3 fats to support mitochondrial membrane integrity; sources include fatty fish, chia seeds, flaxseed, and walnuts.
- Reduce toxic exposure in both diet and environment.
- Exercise regularly, including high-intensity interval training (HIIT), strength training, and aerobic activity. Research supports HIIT as an effective way to improve mitochondrial health.
- Prioritize sleep; deep sleep is when the body repairs and restores cellular function.
- Support gut health and reduce chronic inflammation.
- Address hormone imbalances, particularly thyroid and sex hormones.
- Consider targeted supplementation. CoQ10, acetyl-L-carnitine, alpha-lipoic acid, magnesium, NAC, NADH, D-ribose, and resveratrol have all been studied for their potential to support mitochondrial function.
These are supportive measures and should be paired with proper clinical evaluation, particularly for patients dealing with chronic fatigue, cognitive symptoms, or conditions linked to mitochondrial dysfunction.
How Forum Health Las Colinas Can Help
Our providers use science-based, root-cause protocols to identify and address the factors contributing to mitochondrial dysfunction. Because mitochondrial health intersects with thyroid function, hormone balance, gut health, nutrition, and metabolic health, our evaluations take a comprehensive, whole-body view.
Treatment may include:
- Comprehensive thyroid evaluation and treatment
- Bioidentical hormone replacement therapy
- Gut health testing and treatment
- Nutritional testing and targeted supplementation
- Metabolic and inflammation marker evaluation
- Sleep evaluation and treatment
- Personalized lifestyle and nutritional guidance
For patients in Dallas, DFW, Irving, and Las Colinas dealing with fatigue, cognitive decline, or chronic illness that has not responded to conventional care, a mitochondrial health evaluation is an important and frequently overlooked step toward real answers.
Functional Medicine Performance Health Our Providers
 Start with a Free Phone Consultation
Start with a Free Phone Consultation
If you are experiencing persistent fatigue, brain fog, or symptoms linked to mitochondrial or metabolic dysfunction, our New Patient Coordinator is ready to help.
Contact us for a free phone consultation to learn more about our approach and how we can help you get to the root cause.
Or complete the form below.
Contact Us
"*" indicates required fields
Mitochondrial health is one of the most critical factors in your overall health and energy — yet most people know little about the powerhouse of your cells. However, mitochondria are susceptible and can be damaged easily. And when that damage occurs, you can suffer from fatigue, memory loss, low energy, pain, rapid aging, and much more.
What are Mitochondria?
You may have heard about mitochondria back in biology class, but you may not fully know what they do. Mitochondria are the tiny factories in your cells that take in food and oxygen and convert them into energy. That energy, called ATP (adenosine triphosphate), supports every function of your body. Dr. Mark Hyman, the esteemed functional medicine physician, explains it this way:
“Each cell holds hundreds or thousands of mitochondria; they are found in greater concentrations in active organs and tissues like the heart, brain, and muscles.
“In fact, we have more than 100,000 trillion mitochondria in our bodies, and each one contains 17,000 little assembly lines for making ATP. Mitochondria are where metabolism happens.”
In addition to ATP, mitochondria also produce a byproduct called ROS (reactive oxygen species), which is a type of free radical. These free radicals can damage the mitochondria if you don’t have enough antioxidants in your diet (or make enough in your body).
For More Information on How We Can Help, Call our New Patient Coordinator at 972-960-4800
Or Fill In the Inquiry Form Below, and We Will Contact You!
What Contributes to Mitochondrial Damage?
The natural aging process can contribute to mitochondrial damage, but other things can also contribute. A few examples are stress, lack of sleep, environmental pollution, and eating refined sugar and flour.
Many health issues have been linked to poor mitochondrial function, including:
- Aging
- Cardiovascular disease
- Fibromyalgia
- Skin disorders
- Alzheimer’s disease
- Bipolar disorder
- Infertility
- Depression
- Reproductive problems
- Cancer
- Diabetes
- Fatty liver disease
- Chronic fatigue syndrome
- Inflammatory bowel disease
- Chronic kidney disease
- Insulin resistance
- Multiple sclerosis
- Obesity
- Parkinson’s disease
The reason many issues are related to mitochondrial function is simple: All cellular processes require energy. And a poor energy state is a common denominator in practically all chronic diseases.
That’s why one of the major symptoms of mitochondrial disorders is fatigue — which can have a great deal to do with the thyroid. And the relationship between the thyroid and mitochondria is fascinating.
The Thyroid-Mitochondria Relationship
With damage to the mitochondria comes damage to all your cells — including the thyroid and other hormone-producing cells. However, with thyroid hormones — specifically T3 (triiodothyronine) — the relationship is reciprocal.
T3 affects almost every process in the body and plays a crucial role in your metabolic rate, brain development and function, heart and digestive operations, muscle control, and maintenance of bones. And T3 is also one of the most important regulators of mitochondrial activity — so important that when you remove or reduce T3, mitochondria produce less energy and eventually die.
However, the converse is also true: When your mitochondria are damaged from toxins, chronic stress, or other things that can deplete antioxidants, the thyroid doesn’t produce enough hormones. Then, with reduced thyroid hormones comes a decline in mitochondrial efficiency. It’s a vicious cycle.
That’s why it’s vital to get comprehensive thyroid treatment that uses holistic and standard medical practices to isolate and treat the specific issues with your thyroid. We are experts in thyroid treatment, so to learn more about the thyroid and how we can help get your thyroid right, please visit our Thyroid Treatment page.
Mitochondria and the Gut Microbiome
Your gut is the frontline of defense for your immune system, constantly exposed to toxins, chemicals, pesticide residues, bacteria, and more. And processes in your gut can affect your central nervous system, brain, and moods. But you may not be aware of the gut-mitochondria connection.
In the gut, the cells with their mitochondria and ATP production exist next to the bacteria that make up the gut microbiota. These bacteria interact with the body’s cells mainly through the mitochondria. And studies show that improving the gut microbiome will improve the quality and diversity of the mitochondria’s functions.
However, gut dysbiosis (imbalance of the gut flora) can create a state of chronic inflammation. And this inflammation acts like a constant opposing force on the body’s delicate hormonal balance — and mitochondrial processes essential for energy.
You can learn much more about the importance of a healthy gut microbiome by visiting our Gut Health and Hormones page.
How to Improve Your Mitochondrial Health
- Eat whole foods, mainly plant foods. Vegetables, fruits, nuts, seeds, beans, and whole grains are packed with antioxidants and phytonutrients, so try to eat eight to 12 servings daily.
- Eliminate processed foods, sugar, and junk foods.
- Increase omega-3 fats to help build the mitochondrial membranes. Oily fish like salmon, mackerel, and sardines, plus chia seeds, flaxseed, and walnuts, are all excellent sources.
- Get rid of toxins — both in your body and in your environment.
- Take supplements like acetyl-L-carnitine, alpha lipoic acid, coenzyme Q10, n-acetyl-cysteine, NADH, D-ribose, resveratrol, and magnesium aspartate. These can protect mitochondria and boost energy.
- Get enough sleep. When you sleep well, your body repairs and restores itself, particularly in the deep sleep stage.
- Exercise regularly, doing high-intensity interval training (HIIT), strength training, and aerobic activity. Studies have shown that HIIT training can improve mitochondrial health.
- Balance your hormones. This includes discovering anything that could cause your thyroid hormones to be out of balance.
- Improve your gut health and reduce inflammation.
The offices of Forum Health Las Colinas can Help Discover What May be Damaging Your Mitochondrial Health
Our providers are devoted to understanding your health concerns and symptoms. We use science-based protocols to find the root cause of hormonal imbalances, thyroid dysfunction, nutritional deficiencies, and more.
When it comes to mitochondrial health, as you have read, many issues may be at play. That’s why we will spend quality, personalized time with you to get to the root cause. Treatments may include:
- Bioidentical Hormone Replacement Therapy
- Thyroid Treatment
- Gut Health Testing
- Nutritional Testing
- Sleep Treatment
- And much more
We are here to help you improve your mitochondrial health — and your quality of life!
Contact our New Patient Coordinator for a Free Phone Consultation
Our New Patient Coordinator can explain our protocols and fees in more detail and answer any questions or concerns you have. She can also explain how our approach can help with hormonal balance, anti-aging, and disease prevention to enjoy a vibrant and healthy life!
The health and safety of our staff and patients is a top priority for all of us at the office of Forum Health Las Colinas. We are offering both virtual appointments and in-clinic appointments, whichever you prefer.
If you are coming in to see us in person, keep in mind that we main the highest of standards for the safety of our patients. We sanitize rooms between patient visits and shared surfaces (such as door handles) throughout the day.
Should you choose to have a telemedicine appointment, you will still be able to see your provider, just as if she were standing in front of you in the office. You’ll still get the same “connection” as if your appointment were in the clinic. Additionally, we have mobile phlebotomy services available if you do not want to go to a public lab.
However you choose to have your appointment, we will take the care and time needed to ensure you get all your questions answered. We are here for you!
For More Information, call our New Patient Coordinator at 972-960-4800
Or Fill In the Inquiry Form Below, and We Will Contact You!
"*" indicates required fields

 Eat a whole-food, plant-rich diet high in antioxidants and phytonutrients—vegetables, fruits, nuts, seeds, beans, and whole grains.
Eat a whole-food, plant-rich diet high in antioxidants and phytonutrients—vegetables, fruits, nuts, seeds, beans, and whole grains. Start with a Free Phone Consultation
Start with a Free Phone Consultation

